Research Brief ![]()
Press Release
Download the data
The coronavirus outbreak has had a massive impact on public health and the economy. In the United States, the 25 million workers employed in the service sector have been hit particularly hard by the health and economic crisis. Workers in some segments of the retail and food-service industries have experienced reductions in hours as well as widespread layoffs due to store closures or dramatically reduced demand. At the same time, workers employed in the grocery, delivery, and pharmacy sectors have been designated as “essential” workers and are experiencing an entirely different set of challenges. These workers are continuing to show up to work—stocking shelves, and ringing up and delivering essential food and medicine—risking exposure to a highly contagious and serious illness and facing increased workloads due to co-workers calling out sick.
Before the coronavirus crisis hit, workers in the service sector were already in a precarious position. More than half of these workers lacked access to paid sick leave, and among those who lacked leave, 45% reported they would be unable to deal with a $400 income or expense shock, such as losing a week’s worth of pay while recovering from an illness or caring for loved ones.
The Center for Disease Control has recommended a set of health and safety measures to protect workers on the job. However, federal enforcement of these standards has been weak. The Occupational Safety and Health Administration, the federal agency ordinarily tasked with enforcing regulations to protect workers, has largely left safety standards and protocols up to individual employers.
In this research brief, we draw on survey data collected from about 8,000 workers in March and April 2020 as part of the ongoing Shift Project survey of service-sector workers. This data gives an early and nearly real-time view into employer responses to the COVID-19 pandemic, according to workers. Importantly, we are able to contrast employer responses across different kinds of workplaces, from grocery stores, to fulfillment centers, to fast-food establishments; to chart changes in employer responses over the first weeks of the pandemic; and to focus in on particular employer responses once the scope of the challenge had become clear.
Health and Safety Measures
Overall, we find that 65% of workers surveyed in the five-week period from March 7 to April 9 reported that their workplace had begun requiring employees to do additional cleaning of the store or restaurant. More than half (56%) of workers reported that their employer had made gloves available to workers, but just 19% reported that their employer had made masks available. Much smaller shares reported that their employer had made new requirements for workers to wear gloves or masks (18% and 7%, respectively).
Differences in Health and Safety Across Workplaces
As shown in Figure 1, the reach of these new health and safety measures depends a great deal on the type of workplace. Many workers across workplaces report new cleaning requirements. However, the share ranged from 75% of pharmacy workers to just 26% of delivery workers and 41% of warehouse workers. In more than one-third of grocery stores, coffee shops, fast-food establishments, and restaurants, workers reported that cleaning policies had not changed during the COVID-19 outbreak.
Access to personal protective equipment (PPE) was uneven across sectors. While 72% of workers in hotels and motels and 65% of pharmacy workers reported access to gloves, that was true of under one-third of delivery workers and convenience store workers. Less than half of those in big-box and department stores reported access to gloves, and the share was just over 50% in retail stores, grocery stores, restaurants, fast food, and coffee shops. While we may think of online ordering as a way of avoiding the risks of these brick and mortar locations, just 49% of workers in warehouses and 56% of workers in fulfillment centers reported access to gloves.
Far fewer had access to masks. As with gloves, access was highest in hotels and motels, at 40% of workers, and in pharmacies, at 35%, but the share fell to 4% of fast-food workers, 5% of convenience store and coffee shop workers, and 9% of restaurant workers. About a quarter of workers in retail and grocery stores had access to masks, as did around 15% of those in big-box and department stores. Here, too, the workplaces that back-stop the online economy fell short: just 17% of warehouse, 14% of fulfillment center, and 10% of delivery workers had access to masks.
If access to PPE was limited in our data, policies mandating that workers wear protective gear were even more uncommon. Around a third of workers in restaurants, fast food, coffee shops, and hotels and motels reported requirements to wear gloves. This share was dramatically lower (around 12%) in big-box stores, department stores, retail stores, grocery stores, and pharmacies. The share of workers required to wear gloves was even lower in warehouses, fulfillment centers, and in delivery. Mask requirements were vanishingly uncommon across workplaces, at between 2% and 7% in convenience stores, coffee shops, fast food, restaurants, grocery stores, retail, department stores, and big-box stores. Just 12% of those in fulfillment centers reported a mask requirement, which was significantly higher than the 5% of warehouse and delivery workers.
Change In Health and Safety Over Time
We collected reports from workers between March 7 and April 9 of 2020. We find evidence of significant change in workers’ access to gloves and masks and in employers’ requirements that such PPE be worn. However, even by the end of the first week April, access and requirements to use PPE were uncommon.
Figure 2 shows that at the onset of the survey, in early March, 20% of workers reported new cleaning procedures at their workplaces. This share rose sharply by mid-March to almost 60%, where it has held through early April.
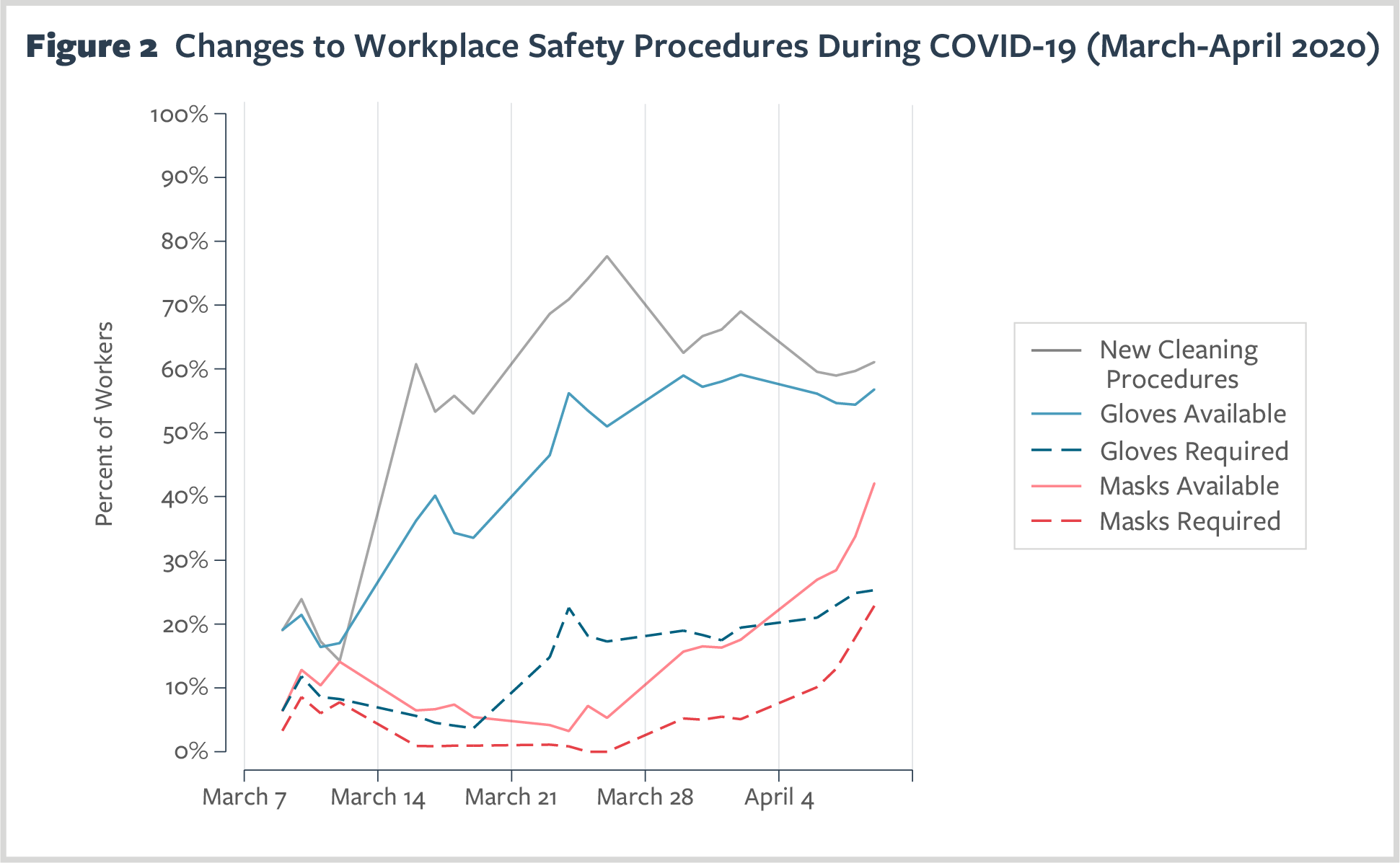
The share of workers reporting access to gloves at work has followed a similar trajectory, rising rather steadily from 20% in early March to over 50% by the end of that month. Access to masks was considerably slower to increase. Mask access was very low (under 10%) at the outset of the survey in early March. These low levels of access continued through the end of March and only began to rise in April, reaching 40% by the end of the first week in April.
Requirements to wear gloves and masks were implemented even more slowly, remaining under 10% through the third week of March, and then only rising to 20% in late March (for gloves) and in early April (for masks).
These plots show evidence that employers first moved to ramp up cleaning, then access to gloves, and then access to masks. However, access to PPE and, especially, requirements to wear PPE, remain very low, with just 50% of workers having access to gloves, 40% access to masks, and only 20% required to wear either by early April, even as the extent and severity of the COVID-19 outbreak was clear by that time.
Employer Variation in Health and Safety
By late March, the true scope and severity of the COIVD-19 outbreak was plain. Yet, we observe significant variation in the extent to which employers had adopted health and safety practices in the period between March 28 and April 9. These next tabulations focus on the subset of companies that we surveyed during this period across five sectors: big box/superstore, grocery, food service (combining fast food and restaurant), warehouse/fulfillment centers, and pharmacy.
Figure 3 shows the percent of workers by company and sector who reported that their employer required additional cleaning of the workplace in response to the coronavirus. Overall, a large share of workers reported additional cleaning requirements, but some companies and sectors were more proactive with than others.
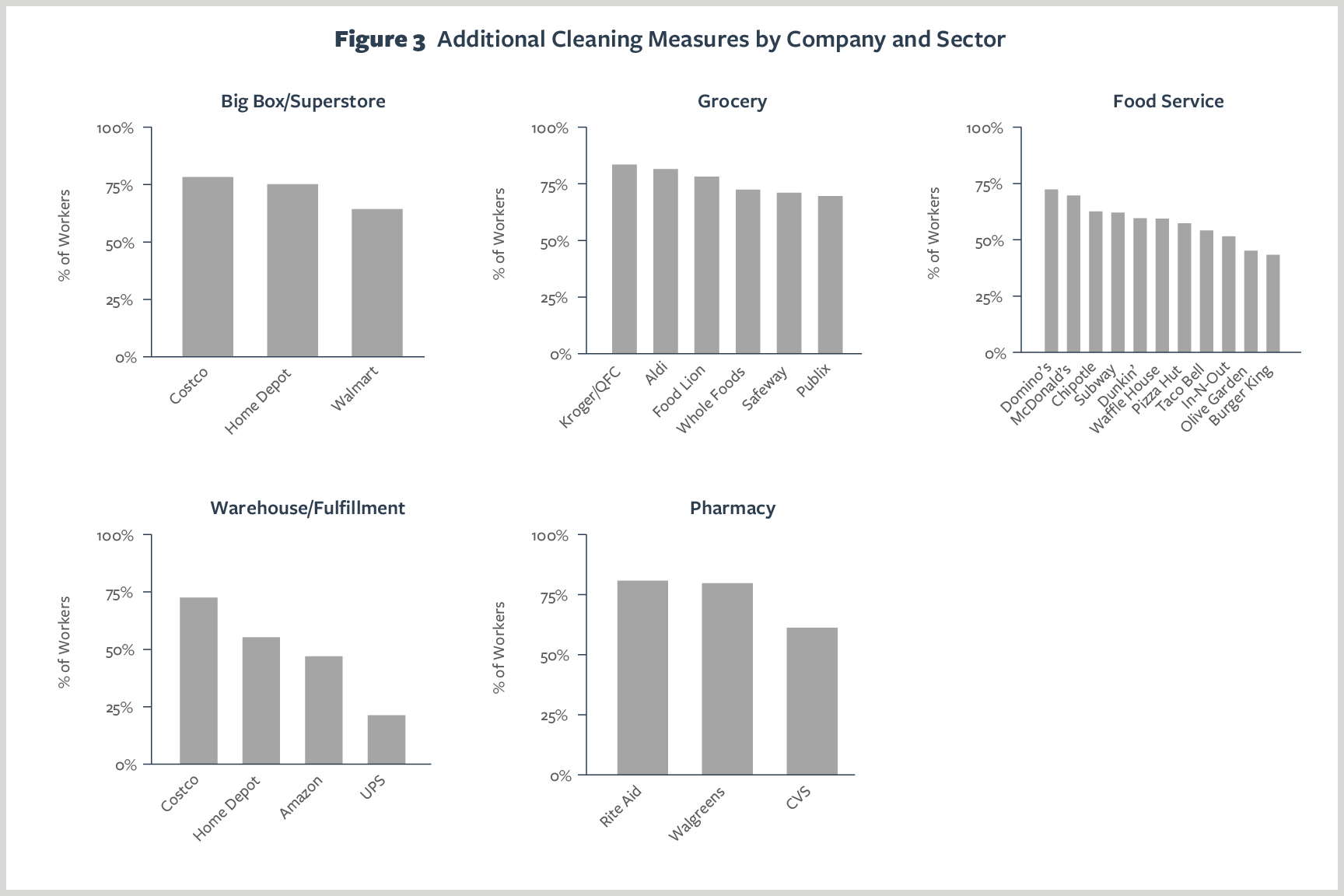
Among big-box stores, at least three-quarters of workers at Costco and Home Depot reported additional cleaning requirements compared with 64% of workers at Walmart. Additional cleaning was slightly more common in the grocery sector, in which Kroger workers were the most likely (84%) and Publix workers were least likely (70%) to report additional cleaning requirements.
There was far more variation in the food-service and warehouse sectors. Among food-service firms, Domino’s and McDonald’s workers were much more likely (70-72%) to report additional cleaning compared with workers at Olive Garden and Burger King (43-45%). In the warehouse/fulfillment sector, almost three-quarters of Costco workers reported additional cleaning, compared with closer to 50% of warehouse workers at Home Depot and Amazon, and only 21% of workers at UPS.
In the pharmacy sector, four out of five Rite Aid and Walgreens workers reported additional cleaning requirements, compared with 61% of workers at CVS.
Figure 4 presents worker reports of the availability of gloves and requirements to wear them in the workplace. In the big-box sector, Costco workers were the most likely to report that gloves were available (83%) and Walmart workers were the least likely (42%). Variation was also wide in the grocery sector, with 95% of workers at Aldi reporting that gloves were available compared with just 47% of workers at Publix. In both of these sectors, requiring gloves was uncommon, with no more than one-third of workers reporting this as a requirement.
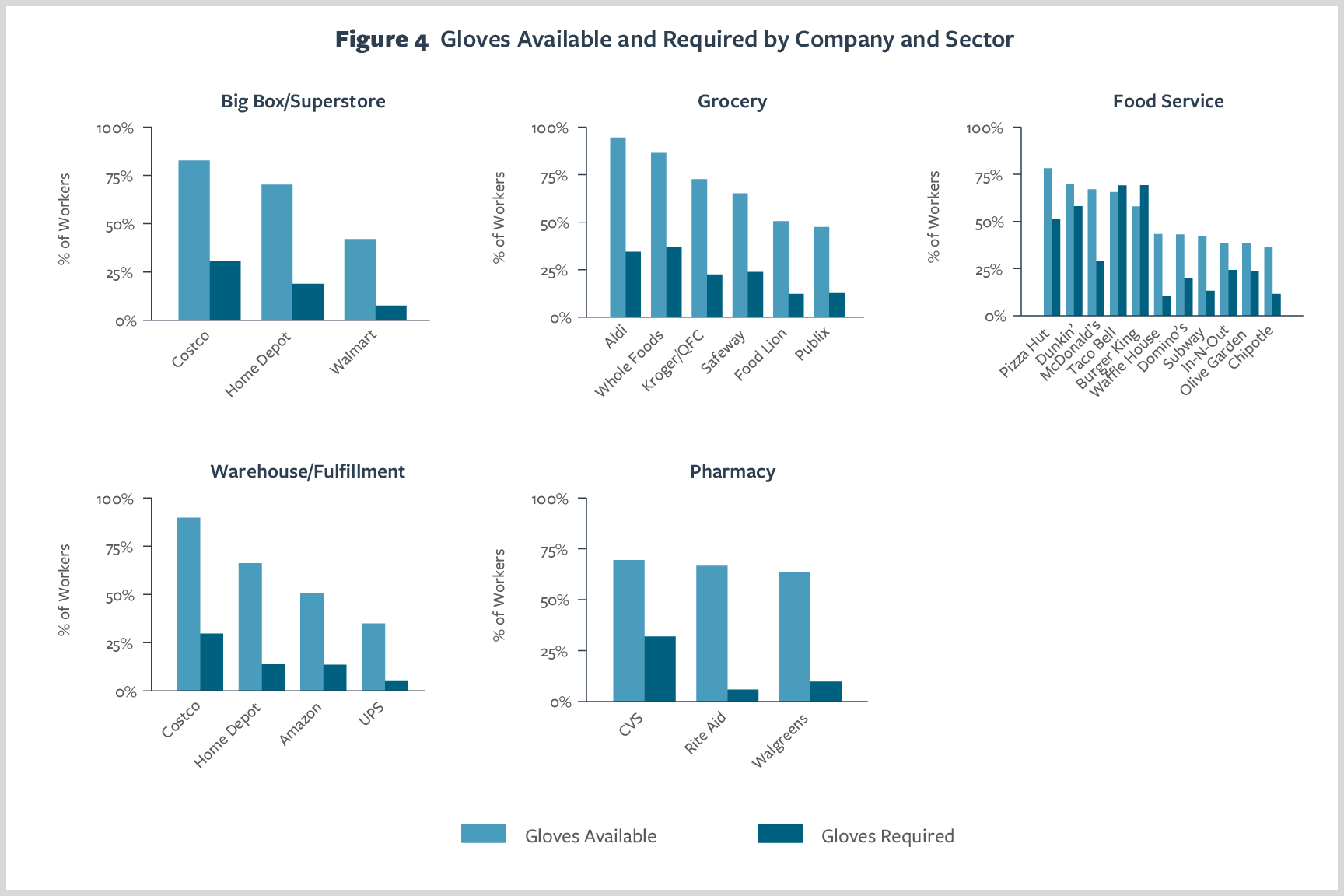
In the food-service sector, availability of gloves ranged from 78% for Pizza Hut workers to just 36% for Chipotle workers. Although the requirement to wear gloves tended to be uncommon, Taco Bell and Burger King stood out, with two-thirds of workers reporting that gloves were required in their workplace.
Among warehouse and fulfillment workers, 90% of Costco workers reported having gloves available, but only 35% of UPS workers did. Amazon fell in between, with 51% of workers reporting that they had gloves available from their employer.
In the pharmacy sector, between 64% and 70% of workers reported having gloves available at work.
Figure 5 shows worker reports of the availability of masks and requirements to use them at work. Overall, masks were far less commonly available than gloves, in spite of the recommendation—and, in some localities, the legal requirement—that masks be worn in public settings such as stores.
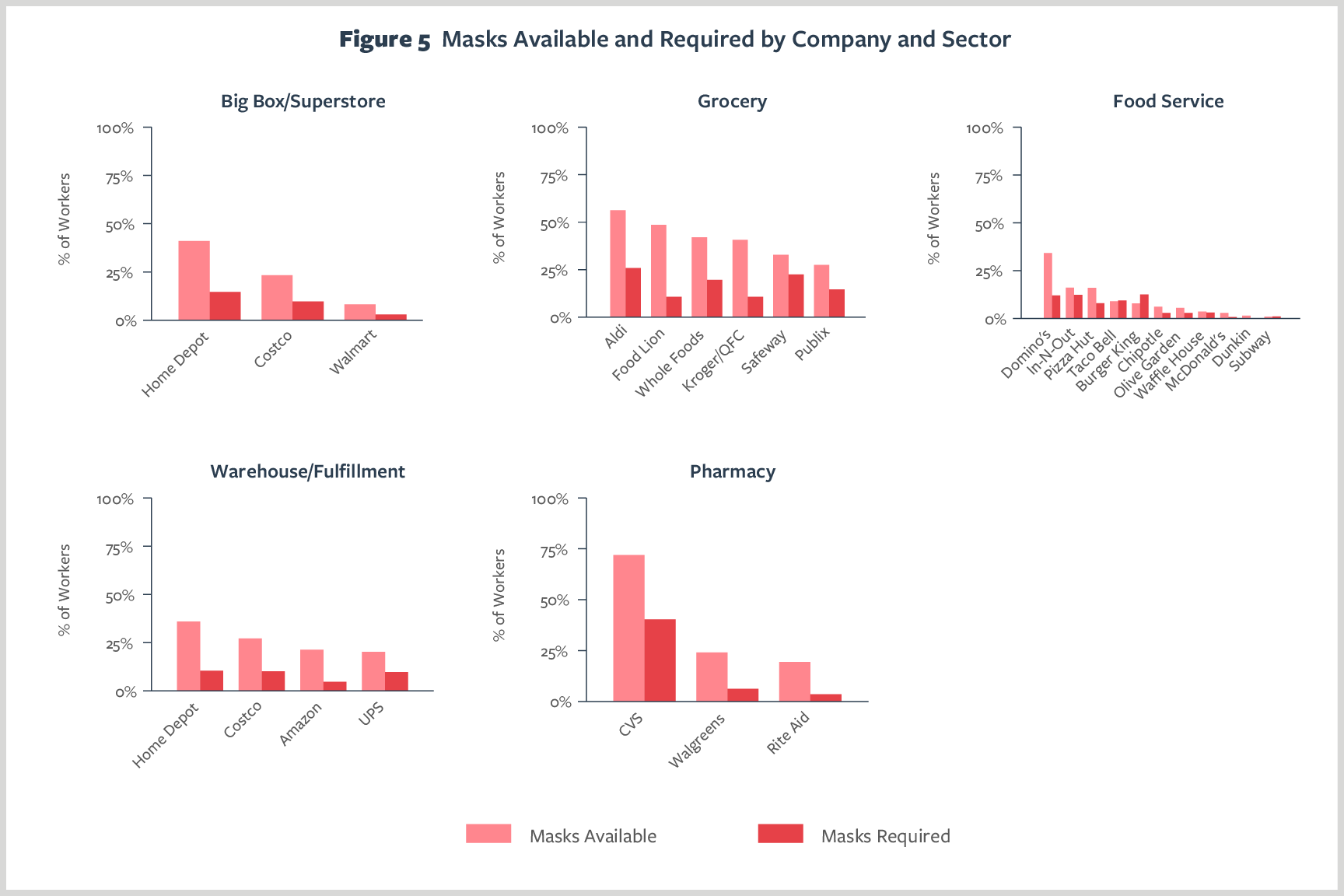
Across sectors and companies, only at CVS (72%) and Aldi (56%) did more than half of workers report that masks were available for them at work. In food service, only Domino’s provided masks for at least one-third of workers. The rest of the food service companies provided masks for only 16% or fewer of workers, and at Subway and McDonald’s almost no workers had masks available.
In late March and early April, employers appeared to be most responsive in requiring additional workplace cleaning, often provided gloves, but rarely provided masks. Requirements to wear gloves or masks were uncommon in most workplaces.
Conclusion
Workers in grocery, big-box stores, pharmacies, food service, and fulfillment are providing the essential services that allow millions of Americans to shelter in place. Effective health and safety measures are needed—to protect the safety of these workers, as well as the safety of customers who venture out to procure food, medicine, and other essential goods.
New data from The Shift Project show that there is a long way to go for employers to ensure that these health and safety needs are being met. This is particularly so in terms of access to PPE like gloves and masks. Over the five-week period from March 7 to April 9, just 18% of workers reported new requirements to wear gloves, and just 7% new requirements to wear masks.
These measures have also been uneven across sectors. Of particular concern, masks were rarely available in food service, grocery, big box, or fulfillment, and access reached above 25% only in hotels and pharmacies, the only sectors where meaningful shares of workers were required to wear masks. While access to gloves is higher, requirements to wear them were also uncommon across sectors, with rates especially low in warehouses, fulfillment centers, and delivery.
At the outset of our survey in early March, additional cleaning as well as access to PPE and requirements to wear PPE was very uncommon. There has been a large increase in cleaning and access to gloves, which rose from 20% of workers to 60% by early April. Requirements to wear gloves also increased, albeit much more slowly, and only reached 20% in early April. Access to masks and requirements to wear masks was near zero through much of March, even as the scope of the pandemic became clear. By early April, 40% of workers reported access to masks, but even then, just 20% reported requirements to wear masks.
The Shift data also show some workplaces were far more proactive than others in instituting additional cleaning and providing masks and gloves to contain the spread of the virus. Among big-box stores and warehouse and fulfillment centers, Costco and Home Depot stand out and Walmart, Amazon, and UPS lag in terms of cleaning, gloves, and masks. In grocery, larger shares of workers at Aldi report cleaning, gloves, and masks, while workers at Publix and Safeway report the fewest new protective measures.
In pharmacy, CVS workers report less new cleaning, but more access to and requirements to use PPE. Health and safety measures are most variable across firms in food service, with the share of workers reporting new cleaning procedures ranging from 75% at McDonald’s to 43% at Burger King, and the share with access to masks ranging from more than a quarter at Domino’s to essentially zero at Subway. Yet, even as there is variation across firms, requirements to wear masks never exceed one-third of workers.
To address these safety shortfalls, Senator Elizabeth Warren and Representative Ro Khana recently proposed a 10-point “essential worker bill of rights.” Their proposal would require that workers have access to necessary protective equipment in their workplaces, stipulates safety procedures when COVID-19 cases occur in a workplace, and would provide hazard pay for workers taking risks to provide essential services.
In the absence of comprehensive federal action, states and localities can play an important role in promoting workplace health and safety and public health. States and localities have the authority to require and enforce safety standards such as cleaning requirements and use of gloves and masks, and to require physical distancing in workplaces.
Until safety standards such as these are strengthened and enforced, workers’ health and safety—and by extension that of the public—are left to the discretion of employers. We find that many employers in front-line industries have been slow to act, and that workers remain underequipped in such vital areas as grocery, fulfillment, food service, and pharmacy.
More frontline worker reports:
- Essential and Vulnerable: Service-Sector Workers and Paid Sick Leave
- Estimates of Workers Who Lack Access to Paid Sick Leave at 91 Large Service Sector Employers
- It’s About Time: How Work Schedule Instability Matters for Workers, Families, and Racial Inequality
- Paid Sick Leave in Washington State: Evidence on Employee Outcomes, 2016–2018
Methodological Appendix
The Shift Project has collected survey data from hourly service sector workers employed at large retail and food establishments since the fall of 2016. This brief focused on a subsample of 8,028 hourly service sector workers employed at 47 of the largest food-service and retail firms who were interviewed between March 7 and April 9, 2020. The survey data collection was national in scope and the survey sample includes respondents from all 50 U.S. states and Washington, D.C. Uniquely, The Shift Project data identify the firm at which each respondent works and contains substantial numbers of respondents at each of the 47 firms described here. The average number of respondents per firm is 171.
The Shift Project recruits survey respondents using online Facebook/Instagram advertisements, targeted to workers employed at large retail and food service employers. Those who responded to the Shift survey invitation were automatically routed to a survey landing page where they were asked to consent to participate in the study, then began the online self-administered survey using the Qualtrics platform. As an incentive, those who completed the survey and provided contact information were entered into a lottery for an Apple iPad. The survey included modules on job characteristics, work schedules, demographics, economic stability, health, parenting, and child outcomes. To screen out invalid survey responses, we used an attention filter (a question that instructed respondents to select a particular response category to verify the accuracy of their responses) as well as a speed filter (discarding data for surveys that were completed too hastily).
The survey recruitment approach yields a non-probability sample of workers, which may differ from the broader population of service sector workers. Therefore, the estimates in this brief may differ somewhat from the broader population of workers. To mitigate this potential bias, we have applied weights that adjust our sample to reflect the universe of service sector workers in the United States. These weights are constructed in two stages.
First, we construct survey weights to adjust the demographic characteristics of the Shift survey sample to match the demographic characteristics of service-sector workers in the American Community Survey (ACS) for the years 2008-2017. We align the ACS sample with the Shift sample by selecting workers in the ACS who are employed in the same occupations and industries as the Shift sample.
Second, to ensure that our sample accurately reflects the distribution of employment types among large retail and food-service employers, we use data from the Reference USA database of U.S. establishments. The RefUSA database contains a detailed listing of all retail and food establishments nationally. RefUSA contains the size of the workforce for each establishment, which we aggregate up to the firm level. Then, using the aggregated RefUSA employer data, we weight our Shift survey sample to match the distribution of workers by firm.
In our analysis of the overall extent of COVID-related health and safety procedures, we estimate weighted (using the combined demographic and employer size weights) unadjusted descriptive statistics. In our analysis of worksite differences in COVID-related health and safety procedures, we present predicted levels from weighted regression models that adjust for age, gender, race/ethnicity, speaking a language other than English at home, having children, union membership, job tenure, and being a manager. In our analysis of change over time, we present weighted three-day moving averages (current period with two lags). In our tabulations of differences by employer, we group employers by the type of worksite at which employees report working and apply the demographic weights, but not the second-stage employment size weight calculated from the RefUSA data.
For a detailed discussion of The Shift Project data collection, methodology, and data validation, see Schneider, D. and K. Harknett. 2019. “What’s to Like? Facebook as a Tool for Survey Data Collection.” Sociological Methods & Research. https://doi.org/10.1177/0049124119882477.
Acknowledgements
The Shift Project gratefully acknowledges funding from the Bill and Melinda Gates Foundation, National Institutes of Health (NICHD), the Robert Wood Johnson Foundation, The James Irvine Foundation, the W.T. Grant Foundation, and support from the Institute for Research on Labor and Employment at UC Berkeley. The views expressed here do not necessarily reflect the official views of the sponsors.
The authors gratefully acknowledge the work of Megan Collins and Connor Williams in the preparation of this report.